Retinal Detachment Surgery: Causes, Procedure, and Effective Treatment Methods
Retinal detachment is a serious condition that can cause vision loss if not treated promptly. It occurs when the retina — the light-sensitive tissue at the back of the eye — separates from the underlying supportive tissue, directly affecting the eye’s ability to see. One of the effective treatments to address this condition is retinal detachment surgery.
In this article, we will explore the causes of retinal detachment, the signs to watch for, the surgical procedure, and important considerations during recovery. This information is provided clearly and accurately to help you better understand the condition and make informed decisions about treatment.
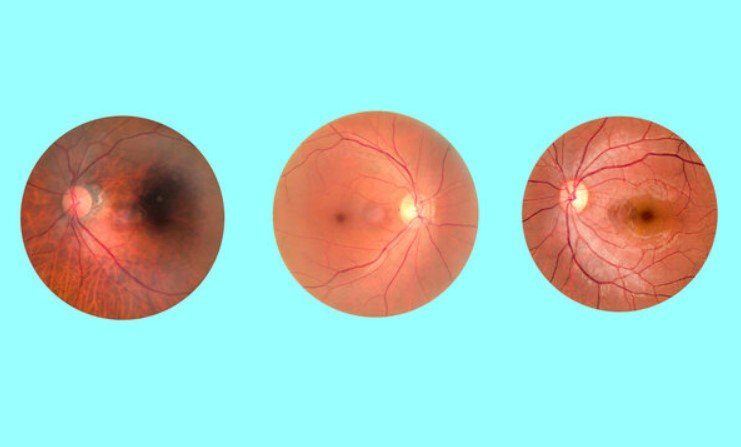
What is Retinal Detachment Surgery?
Retinal detachment surgery is a medical procedure performed to treat retinal detachment, where the retina — the light-sensitive layer at the back of the eye — separates from the underlying tissue. Without timely treatment, retinal detachment can lead to permanent vision loss.
The surgery aims to reposition the retina back to its original location and secure it using various techniques such as gas injection, liquids, or laser treatment. This procedure is crucial to prevent permanent damage to vision, especially in severe cases or those with a high risk of blindness.
Retinal detachment can occur without clear warning signs, so regular eye exams are the best way to detect early abnormalities in the retina.
Causes of Retinal Detachment
Retinal detachment can occur due to various causes, including:
- Eye trauma: Accidents or strong impacts to the eye can cause the retina to tear or detach from the underlying tissue.
- Eye diseases: Conditions such as high myopia (severe nearsightedness), diabetes, or endophthalmitis can increase the risk of retinal detachment. These conditions may cause structural and functional changes in the retina, leading to detachment.
- Aging: The natural aging process can weaken the retinal connective tissue, increasing the risk of retinal detachment, especially in older adults.
- Glaucoma: Elevated intraocular pressure can damage the eye and cause retinal detachment.
- Genetics: Some individuals have a higher risk of retinal detachment if there is a family history of the condition.
- Other diseases: Conditions such as ocular tumors, retinitis, or disorders that reduce blood supply to the eye can also lead to retinal detachment.
Retinal detachment is a serious medical condition that requires timely treatment to protect vision.
>> Retinal diseases in older adults, such as macular degeneration, can cause serious damage to the back of the eye and require close monitoring.
Signs and Symptoms of Retinal Detachment
Retinal detachment is a severe condition that can cause permanent vision loss if not detected and treated promptly. Below are some common signs and symptoms:
- Sudden blurred vision: One of the most noticeable symptoms is sudden blurring or loss of vision, usually in one eye.
- Seeing a “veil” or blind spots: Patients may feel as if a veil or curtain is covering their vision or notice blind spots, making it difficult to see clearly.
- Flashes of light and seeing “sparkles”: Some people experience flashes or flickering lights in their vision, especially when moving or changing lighting conditions.
- Increased number of floaters: Floaters are small dark spots or threads drifting in the field of vision. A sudden increase in floaters can be a warning sign of retinal detachment.
- Loss of peripheral vision: Retinal detachment may affect side vision, making it difficult to see objects at the edges of the visual field.
If you experience any of these symptoms, consult an eye specialist immediately for examination and timely treatment. Early detection is crucial to prevent serious vision damage.
>> Premature infants with retinopathy of prematurity (ROP) require close monitoring due to a high risk of retinal detachment during early development.
Surgical Methods for Retinal Detachment
Surgery is necessary to restore the retina to its original position when it detaches from the underlying tissue. There are several surgical methods used, depending on the patient’s condition. The most common methods include:
Pneumatic Retinopexy
This method involves injecting a gas bubble into the eye to help push the retina back into place. The doctor then uses laser or cryotherapy (freezing) to seal the retina to the underlying tissue. Pneumatic retinopexy is suitable for mild cases of retinal detachment with few tears.
Vitrectomy
This surgery involves removing part of the vitreous gel (the clear gel filling the eye) to create space and allow the retina to be repositioned. The doctor may use gas or silicone oil to hold the retina in place and apply laser treatment to ensure the retina reattaches fully. Vitrectomy is indicated for more complex retinal detachment cases.
>> In some cases, vitrectomy surgery is performed alongside retinal detachment treatment or when retinal detachment occurs due to vitreoretinal traction.
Scleral Buckling
This procedure involves placing a silicone band or other soft material around the outside of the eye to indent the eye wall and support the retina’s reattachment. This method helps prevent recurrent retinal detachment. Scleral buckling is often performed when there is a large retinal tear or detachment caused by trauma.
Each surgical method has its own advantages and limitations. The choice of technique depends on the specific condition of the patient, as assessed by the ophthalmologist.
Retinal Detachment Surgery Procedure
Retinal detachment surgery is a complex procedure that must be performed by an experienced eye specialist. The surgical process includes the following steps:
Preoperative Preparation
- Clinical Examination: The doctor conducts a thorough eye examination, including refractive error measurement, retinal evaluation, and assessment of the detachment severity.
- Imaging Diagnosis: Techniques such as Optical Coherence Tomography (OCT) or fundus photography are used to get a detailed view of the retina and help decide the best surgical approach.
- Consultation: The doctor explains the surgical procedure, possible risks, and discusses the next steps with the patient.
Anesthesia
Retinal detachment surgery is usually done under local anesthesia. The patient receives anesthetic eye drops or injections around the eye to ensure no pain during the operation.
Surgical Procedure
- Vitrectomy: The surgeon removes part of the vitreous gel to access the retina and remove any factors affecting recovery.
- Retina Reattachment: Depending on the detachment, the doctor uses gas, silicone oil, or scleral buckling to reposition the retina.
- Laser or Cryotherapy: After repositioning, laser or freezing treatment is applied to fix the retina firmly in place.
Completion
- After the surgery, the doctor checks the eye to ensure stability.
- The patient is moved to the recovery room for postoperative monitoring. Mild eye discomfort or fatigue is common during this period.
Postoperative Care Instructions
- The doctor provides guidelines on eye care after surgery, including the use of eye drops, avoiding touching the eye, and attending follow-up examinations.
- Recovery time varies depending on the surgery complexity. Patients need patience and strict adherence to medical advice for the best outcomes.
Retinal detachment surgery is a critical procedure that should be performed at reputable medical facilities. Early detection and timely treatment are essential for effectively preserving vision.
Recovery Time After Retinal Detachment Surgery
The recovery time after retinal detachment surgery can vary depending on the individual patient, the surgical method used, and the severity of the detachment. However, below are common recovery milestones and general factors patients can refer to:
Immediately After Surgery
- Recovery Room Monitoring: After surgery, patients are taken to the recovery room for health monitoring. This period usually lasts from a few hours up to one day.
- Temporary Discomfort: Patients may experience mild eye pain, blurred vision, or a feeling of heaviness in the eye during the first few days post-surgery.
First Week
- Postoperative Check-up: The doctor will schedule a follow-up visit within one week after surgery to evaluate the healing process and address any complications.
- Activity Restrictions: Patients are advised to avoid strenuous activities, heavy lifting, and rubbing the eyes.
- Medications and Eye Care: Use of prescribed eye drops to reduce inflammation and prevent infection is essential. Mild pain relievers may also be recommended in the early days after surgery.
1 to 4 Weeks After Surgery
- Vision Improvement: Vision may gradually improve, but patients may still experience some blurriness or light sensitivity during this phase.
- Follow-up Examinations: Continued monitoring by the ophthalmologist to assess recovery and surgical outcomes.
- Avoid Eye Exposure to Water: Patients should avoid getting water or dust into the eye for several weeks to minimize infection risk.
2 to 3 Months After Surgery
- Stabilizing Vision: Significant improvement in vision may occur during this period, although full recovery might take longer to achieve optimal results.
- Reduction in Discomfort: Symptoms like blurred vision or eye heaviness typically decrease gradually.
6 Months to 1 Year After Surgery
- Complete Recovery: For many patients, vision stabilizes and recovers fully within 6 months to 1 year after surgery. However, some cases may require additional treatments or long-term monitoring.
- Regular Follow-ups: Patients should continue regular check-ups to monitor eye health and detect any emerging issues early.
Important Notes:
- Recovery time varies from case to case. Some patients recover quickly, while others may require a longer time for full healing.
- Strictly following the doctor’s instructions regarding eye care, medication use, and health monitoring enhances recovery chances and reduces the risk of complications.
Retinal detachment surgery is a complex procedure, but with proper surgical technique and postoperative care, patients can effectively restore vision and lower the risk of recurrence.
Possible Complications After Retinal Detachment Surgery
Although retinal detachment surgery is an effective treatment for repairing retinal detachment, like any surgical procedure, it carries some risks of complications. These complications may affect the recovery process and the final surgical outcome. Below are some common complications that can occur after retinal detachment surgery:
Infection
- Despite strict sterilization measures by surgeons, infections can still occur post-surgery. Infection may lead to endophthalmitis (eye inflammation), pain, and even vision loss if not treated promptly.
- Prevention: Use prescribed antibiotic eye drops and maintain careful eye hygiene.
Intraocular Bleeding
- Some patients may experience bleeding inside the eye after surgery. This may result from minor damage during the procedure or changes in blood flow postoperatively.
- Prevention: Regular eye examinations and adherence to prescribed medications to reduce bleeding risk.
Recurrent Retinal Detachment
- Although the surgery aims to reattach the retina, the retina may detach again in some cases, especially if postoperative care instructions are not followed properly.
- Prevention: Close monitoring and strict compliance with the surgeon’s postoperative care instructions.
Blurred Vision or Decreased Visual Acuity
- Patients may experience temporary blurred vision or reduced vision following surgery, which can be a reaction to structural changes in the eye.
- Prevention: Regular follow-ups and patience during the healing process as vision may gradually improve.
Increased Intraocular Pressure (Glaucoma)
- Elevated eye pressure may develop after surgery, particularly if corticosteroids are used during treatment. Uncontrolled high pressure can damage the optic nerve.
- Prevention: Routine intraocular pressure measurements as recommended to detect and manage elevated pressure early.
Scar Formation in the Retina
- Scar tissue may develop within or around the surgical site, potentially affecting vision.
- Prevention: Timely monitoring and treatment if signs of scarring appear.
Cataract Formation
- In some cases, retinal detachment surgery can lead to cataract development (clouding of the lens), especially if the surgery involves deeper intervention inside the eye.
- Prevention: Regular check-ups to detect early cataract signs and appropriate treatment when necessary.
Although complications may arise after retinal detachment surgery, most can be effectively managed with proper care and regular monitoring. It is crucial for patients to fully follow their doctor’s instructions on eye care and attend scheduled follow-up appointments to ensure smooth recovery.
Postoperative Eye Care After Retinal Detachment Surgery
Proper eye care after retinal detachment surgery is crucial to ensure optimal recovery and minimize the risk of complications. Here are important guidelines to help you care for your eyes following the procedure:
- Follow Your Doctor’s Instructions
The most important step is to strictly follow all medical advice regarding the use of prescribed eye drops, oral medications, and eye care measures. This helps reduce infection risk and control intraocular pressure. - Use Medications as Directed
After surgery, your doctor will prescribe antibiotic and anti-inflammatory eye drops or oral medicines. Use these medications correctly and consistently to ensure effectiveness. - Avoid Trauma or Pressure to the Eye
In the first days after surgery, avoid rubbing your eyes or any strong impact, as this can damage the healing retina. - Rest and Limit Eye Strain
Allow your eyes and body adequate rest. Avoid prolonged activities that strain the eyes, such as watching TV, reading, or using digital devices excessively, since this may increase eye pressure. - Minimize Exposure to Water
Avoid getting water in your eyes during the first week post-surgery. Limit activities like bathing in tubs, swimming, or washing your face directly with water to prevent infection. - Protect Your Eyes from Bright Light
Eyes may be sensitive to light after surgery. Wear UV-protected sunglasses outdoors to shield your eyes from strong sunlight. - Avoid Heavy Physical Activities
Refrain from strenuous exercise, lifting heavy objects, or vigorous movements for a period to reduce pressure on your eyes. - Attend Regular Follow-Up Appointments
Scheduled check-ups allow your doctor to monitor healing progress and detect any early complications, adjusting treatment as needed. - Watch for Warning Signs
If you experience severe pain, sudden vision loss, bleeding, or persistent blurred vision after surgery, seek immediate medical attention.
Proper postoperative eye care plays a vital role in ensuring successful recovery after retinal detachment surgery. By following your doctor’s instructions carefully and maintaining good eye hygiene, you protect the surgical outcome and support long-term eye health.
Retinal detachment surgery is an important procedure to restore vision in patients with retinal tears or detachment. Careful eye management afterward helps ensure smooth healing and reduces complication risks. Use all prescribed medications, avoid eye trauma, get enough rest, and keep your follow-up appointments to monitor progress.
If you have any questions or notice unusual symptoms, don’t hesitate to contact your eye specialist for timely advice and support. Proper eye care not only protects your vision but also improves your overall quality of life.