Diabetic Retinopathy: Causes, Symptoms, Stages, and Treatment Options
Table of Contents
Diabetic retinopathy is one of the most serious complications of diabetes, directly affecting vision and potentially leading to blindness if not detected and treated promptly. This condition occurs when prolonged high blood sugar levels damage the blood vessels in the retina, reducing visual clarity. In this article, we’ll explore the causes, symptoms, developmental stages, and treatment options for diabetic retinopathy to help you better protect your eye health—especially if you are living with diabetes.
What is Diabetic Retinopathy?
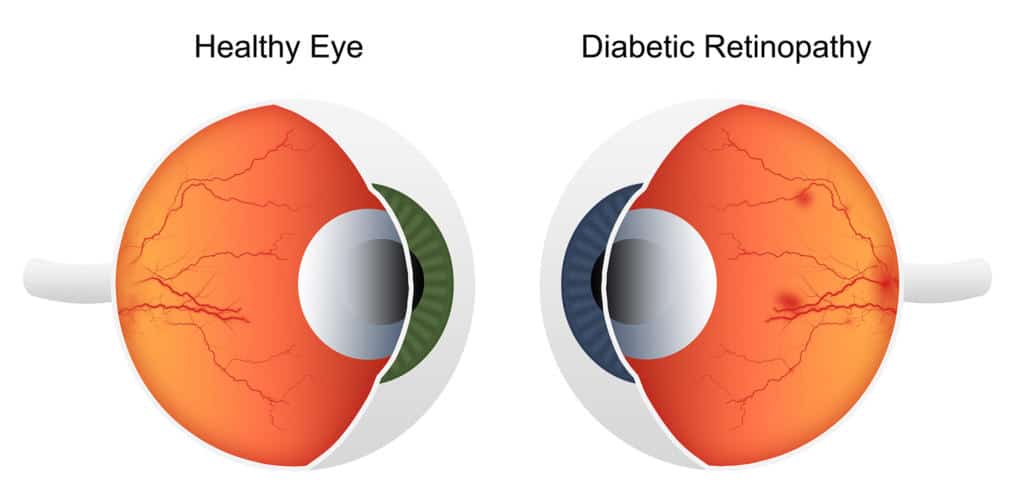
Diabetic retinopathy is a serious diabetes-related eye disease that occurs when chronically elevated blood glucose levels damage the small blood vessels in the retina—the light-sensitive tissue at the back of the eye. If left untreated, diabetic retinopathy can result in vision loss or even permanent blindness.
When the retinal blood vessels are damaged, they may leak fluid or blood, causing swelling and impairing retinal cells. This directly affects your ability to see clearly. That’s why maintaining good blood sugar control and scheduling regular eye exams are critical for individuals with diabetes.
Causes of Diabetic Retinopathy
The main cause of diabetic retinopathy is prolonged high blood sugar (hyperglycemia) in individuals with diabetes. Poor blood sugar control over time can weaken and damage the tiny blood vessels that nourish the retina, leading to leakage and inflammation. Below are the key risk factors contributing to the development of diabetic retinopathy:
Prolonged High Blood Sugar
Chronic hyperglycemia is the most significant cause of retinal blood vessel damage. Over time, high blood sugar weakens the vessel walls, making them more likely to rupture or leak, which leads to retinal damage.
High Blood Pressure
Hypertension increases pressure on blood vessels throughout the body, including the eyes. In people with diabetes, elevated blood pressure significantly raises the risk and progression of diabetic retinopathy.
Duration of Diabetes
The longer a person has diabetes (especially over 10 years), the higher the risk of developing diabetic retinopathy. Long-term exposure to high blood sugar increases cumulative damage to the retina.
Dyslipidemia (Abnormal Blood Lipid Levels)
A diet high in saturated fat and cholesterol can increase the risk of damage to the retinal blood vessels. Elevated levels of blood lipids can accelerate the onset and progression of diabetic eye disease.
Genetics
A family history of diabetes or diabetic retinopathy may increase your personal risk. Genetic predisposition plays a role in how susceptible your eyes are to diabetes-related complications.
Understanding the causes of diabetic retinopathy empowers you to take proactive steps in managing your diabetes and reducing your risk of vision-threatening complications.
Symptoms of Diabetic Retinopathy
Diabetic retinopathy can develop silently and may not show noticeable symptoms in its early stages. However, as the condition progresses, certain symptoms may appear and affect vision. Below are the most common signs of diabetic retinopathy:
- Blurred vision
One of the most common symptoms of diabetic retinopathy is blurred vision, especially in low-light conditions or while reading or driving. This occurs due to damage to the retinal blood vessels, making it difficult for images to be clearly transmitted to the brain. - Floaters or dark spots in vision
Patients may notice dark spots, shadows, or floaters in their field of vision. These are caused by blood or fluid leaking from damaged blood vessels into the retina. - Gradual loss of peripheral vision
Diabetic retinopathy can reduce peripheral (side) vision, making it difficult for patients to see objects outside their direct line of sight. - Difficulty seeing in low light
Patients may struggle to see clearly in dim environments, such as driving at night. This is a sign that the retina is significantly affected. - Blurry vision when changing focus
Vision may become temporarily blurred when shifting gaze suddenly, especially when looking up or down. - Eye bleeding or cloudy vision
In advanced stages, diabetic retinopathy can cause intraocular bleeding, leading to blurry or clouded vision. In some cases, this may result in temporary vision loss.
If you experience any of these symptoms—especially if you have diabetes—you should consult an eye specialist immediately. Early detection and timely treatment of diabetic retinopathy can help preserve long-term vision.
>> Although diabetic retinopathy and cataracts are two different conditions, people with diabetic retinopathy are at higher risk of developing cataracts.
Stages of Diabetic Retinopathy
Diabetic retinopathy progresses through several stages, from early signs to severe complications that may threaten vision. Understanding these stages helps patients detect the condition early and seek timely treatment. The stages include:
Stage 1: No apparent retinopathy (Hidden stage)
At this stage, there are no noticeable symptoms. Blood vessels in the retina may be damaged without affecting vision. Routine eye exams are crucial, especially for individuals with diabetes, to detect early retinal changes.
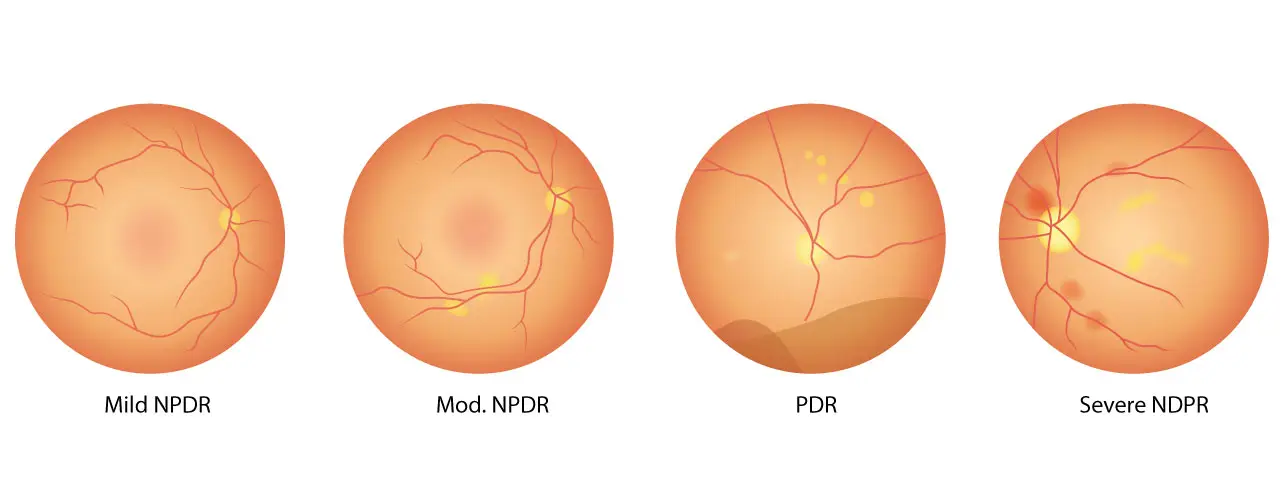
Stage 2: Non-proliferative diabetic retinopathy (NPDR)
This early stage involves weakening of the retinal blood vessels, which may leak fluid or blood. Vision is often not significantly affected yet. However, if left untreated, the disease can progress rapidly.
Stage 3: Proliferative diabetic retinopathy (PDR)
In this more advanced stage, severely damaged blood vessels trigger the growth of new, fragile vessels (neovascularization). These abnormal vessels are prone to bleeding, causing severe vision loss. This stage can lead to blindness if not treated promptly.
Stage 4: Diabetic macular edema (DME)
DME is a common complication of advanced diabetic retinopathy. Damaged blood vessels leak fluid into the macula—the central part of the retina—causing swelling and blurred central vision. Without timely treatment, it can cause permanent vision damage.
Each stage of diabetic retinopathy requires proper monitoring and treatment. Early diagnosis and intervention can reduce the risk of complications and protect long-term eye health.
In some severe cases of retinopathy, patients may require retinal detachment surgery to preserve their vision.
Treatment Options for Diabetic Retinopathy
Treatment for diabetic retinopathy depends on the stage and severity of retinal damage. The main goals are to slow disease progression, minimize retinal damage, and preserve vision. Common treatment options include:
Blood sugar control
Managing blood glucose is the most crucial part of diabetic retinopathy treatment. Maintaining stable blood sugar levels can prevent the disease from worsening and protect the retinal blood vessels. Patients should follow a balanced diet, take medications as prescribed, and monitor their glucose regularly.
Laser treatment (Laser photocoagulation)
Laser therapy is used for advanced cases, especially in proliferative diabetic retinopathy (PDR). Laser photocoagulation seals leaking blood vessels, reduces retinal bleeding, and may help manage macular edema to prevent vision loss.
Anti-VEGF injections
Intravitreal injections of anti-VEGF (vascular endothelial growth factor) medications such as ranibizumab (Lucentis) or aflibercept (Eylea) are effective treatments, especially for diabetic macular edema. These drugs reduce abnormal blood vessel growth and fluid leakage, improving visual outcomes.
Vitrectomy surgery
This surgical procedure is indicated in severe cases, particularly when there is vitreous hemorrhage or retinal detachment. Vitrectomy removes blood, scar tissue, and damaged vitreous gel to restore vision and prevent further retinal damage.
Combination treatment
In some cases, ophthalmologists may recommend a combination of therapies such as laser surgery, anti-VEGF injections, and blood sugar control to achieve the best results.
Treatment should always be guided by a qualified eye specialist. Early intervention is key to preventing serious complications, preserving vision, and improving quality of life for patients with diabetic retinopathy.
How to Prevent Diabetic Retinopathy
Diabetic retinopathy is one of the most serious complications of diabetes and can lead to permanent vision loss if not detected and treated in time. However, the disease is highly preventable and its progression can be slowed with proper diabetes management and healthy lifestyle choices. Below are effective ways to help prevent diabetic retinopathy and protect your eyesight:
- Maintain Stable Blood Sugar Levels
Keeping your blood glucose levels within the target range is the most critical factor in preventing diabetic retinopathy. Follow a diabetes-friendly diet, take medications or insulin as prescribed, and monitor your blood sugar regularly to prevent spikes that can damage the retina. - Schedule Regular Eye Exams
Annual comprehensive eye exams are essential for early detection of diabetic retinopathy. People with diabetes should see an ophthalmologist or retina specialist at least once a year to check for early signs of retinal damage. Early diagnosis significantly improves treatment outcomes and can prevent vision loss. - Maintain a Healthy Weight
Being overweight increases the risk of diabetes complications, including diabetic retinopathy. Achieving and maintaining a healthy body weight through a balanced diet and regular exercise can help control blood sugar and reduce the risk of eye damage. - Follow a Balanced and Eye-Healthy Diet
A nutrient-rich diet supports both blood sugar control and eye health. Limit sugary and processed foods, and include more whole grains, leafy greens, fruits, nuts, and foods high in vitamins A, C, and E, which support retinal function and protect blood vessels in the eyes. - Exercise Regularly
Engaging in moderate physical activity—such as walking, jogging, swimming, or yoga—for at least 30 minutes a day can help regulate blood glucose levels and improve overall vascular health. Regular exercise is also linked to reduced progression of diabetic eye disease. - Control Blood Pressure and Cholesterol
High blood pressure and elevated cholesterol levels contribute to damage of the tiny blood vessels in the retina. Managing these conditions through lifestyle changes and/or medication is an essential part of preventing diabetic retinopathy. - Avoid Smoking and Limit Alcohol Consumption
Smoking and excessive alcohol intake can accelerate blood vessel damage and increase the risk of diabetic eye disease. Quitting smoking and limiting alcohol are key steps toward protecting your vision and overall health.
Diabetic retinopathy is a serious but preventable complication of diabetes. By maintaining good blood sugar control, adopting a healthy lifestyle, and having your eyes examined regularly, you can significantly lower your risk of developing vision-threatening complications.
If you have diabetes, make sure to follow your doctor’s guidance and take proactive steps to care for your eyes. Early detection and proper eye care are the keys to long-term vision protection.

5 Things to Know Before Traveling Abroad for Eye Surgery
When it comes to eye surgery, many patients are exploring the option of traveling abroad for treatment. Eye surgeries like

Prosthetic Contact Lenses: A Personalized Solution for Vision and Confidence
If you have an eye injury, visible iris defect, or a condition that affects the appearance or function of your
Common Retinal Diseases and Effective Prevention Methods
The retina, a thin and sensitive layer of nerve tissue at the back of the eye, plays a pivotal role

How to Stop Eye Twitching: Causes and Effective Remedies
Eye twitching, or an eyelid twitch, is a common phenomenon almost all of us have experienced at least once. Sometimes

How to Read Your Eyeglass Prescription: A Simple Guide from A to Z
Just visited your eye doctor and received a piece of paper filled with numbers and symbols that look complicated? Don’t