
20/20 Vision: The Gold Standard for Sight and How to Achieve Healthy Eyes
In the world of ophthalmology, 20/20 vision is a familiar term, often considered the gold standard for healthy eyes. But
Glaucoma is a group of eye diseases that damage the optic nerve, often caused by increased pressure inside the eye. It is one of the leading causes of irreversible blindness worldwide. Early stages of glaucoma usually show no symptoms, making regular eye exams essential for timely diagnosis and effective management. Understanding the causes, symptoms, and available treatment options can help protect your vision and improve quality of life. This guide also highlights the latest research, factors influencing treatment decisions, and where to find expert glaucoma care and eye doctors in Ho Chi Minh City, Vietnam.
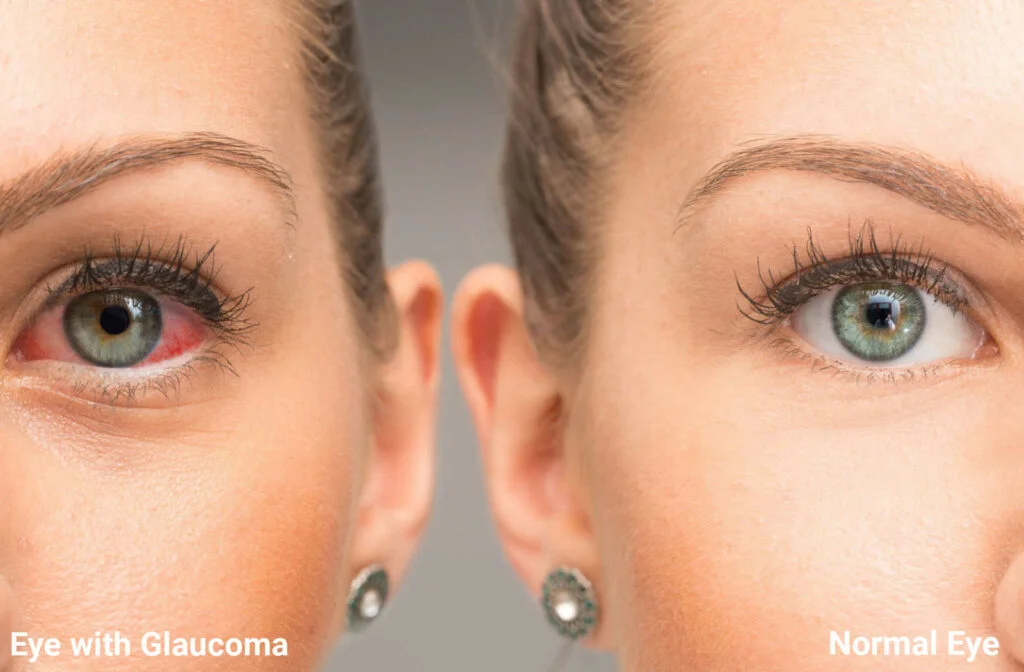
Glaucoma is a chronic eye condition characterized by damage to the optic nerve, which is vital for transmitting visual information from the eye to the brain. This damage is often linked to elevated intraocular pressure (IOP), although glaucoma can also occur with normal eye pressure.
The most common cause of glaucoma is increased fluid buildup inside the eye, which raises intraocular pressure and damages the optic nerve over time. There are different types of glaucoma, including:
Glaucoma is one of the common eye diseases that affect older adults, alongside age-related macular degeneration.
Glaucoma is often called the “silent thief of sight” because it usually develops without noticeable symptoms in its early stages. As the disease progresses, symptoms may include:
Certain factors increase the risk of developing glaucoma:
Because early glaucoma symptoms are often absent, regular comprehensive eye exams are critical for early detection and prevention of vision loss.
>> People with diabetes are at high risk of developing multiple eye diseases such as diabetic retinopathy and glaucoma, and require careful monitoring to protect long-term vision.
Effective management of glaucoma focuses on lowering intraocular pressure (IOP) to prevent further damage to the optic nerve and preserve vision. Treatment choices depend on the type and severity of glaucoma, as well as the patient’s overall health.
Eye drops are the most common first-line treatment to reduce eye pressure. Different classes of medications work by either decreasing the production of aqueous humor (eye fluid) or improving its drainage. Common types include:
Patients must use these medications consistently as prescribed, and regular follow-up visits are essential to monitor effectiveness and side effects.
Laser therapy can improve fluid drainage and reduce eye pressure, often used when medications are insufficient or to delay surgery. Types of laser treatments include:
When medications and laser therapy do not adequately control glaucoma, surgical options may be considered. Surgery aims to create a new drainage pathway to lower intraocular pressure. Common procedures include:
In addition to medical treatment, patients with glaucoma benefit from regular eye exams to track disease progression. Maintaining a healthy lifestyle, managing systemic conditions like diabetes and hypertension, and avoiding activities that significantly raise eye pressure can also help.
Choosing the right treatment depends on multiple factors, including glaucoma type, stage, and patient preferences. Working closely with an experienced eye doctor ensures personalized care and optimal outcomes.
>> In some patients, angle-closure glaucoma may be accompanied by cataracts. In such cases, cataract surgery not only improves vision but also helps lower intraocular pressure.
Glaucoma management is continually evolving with advances in medical research and technology aimed at improving treatment effectiveness and preserving vision. Recent developments focus on innovative therapies that offer hope for better disease control and fewer side effects.
Researchers are developing novel medications targeting different pathways involved in eye pressure regulation and optic nerve protection. Some promising drugs include:
MIGS techniques continue to advance, offering safer surgical options with faster recovery times. These procedures involve tiny implants or devices that improve eye fluid drainage with minimal tissue disruption. Examples include the iStent, Hydrus Microstent, and Xen Gel Stent. MIGS is increasingly preferred for early to moderate glaucoma cases.
Cutting-edge studies are exploring gene therapy to correct genetic factors that cause glaucoma, as well as stem cell therapy to regenerate damaged optic nerve tissue. While still largely experimental, these approaches represent potential future breakthroughs for restoring vision lost to glaucoma.
Innovations in home-monitoring technology allow patients to track their intraocular pressure regularly outside the clinic. Devices like implantable sensors and wearable tonometers improve disease management by providing real-time data for both patients and doctors.
AI-powered tools are increasingly used to analyze retinal images and visual field tests, improving early detection and personalized treatment planning. AI helps identify subtle changes that may be missed by conventional exams, enabling timely intervention.
Ongoing research and clinical trials are vital to advancing glaucoma care. Patients should consult with their eye specialists about new treatment options and clinical trial opportunities suitable for their condition.
Choosing the most appropriate treatment for glaucoma depends on multiple individual factors. Eye care specialists consider these aspects to tailor the management plan for each patient, ensuring the best possible outcomes while minimizing risks.
The specific type of glaucoma—such as open-angle, angle-closure, or normal-tension glaucoma—significantly affects treatment decisions. Early-stage glaucoma may be managed effectively with medications or laser therapy, while advanced cases might require surgical intervention to better control intraocular pressure.
Treatment intensity often depends on the patient’s current eye pressure and target pressure to prevent optic nerve damage. Patients with very high IOP may need more aggressive treatment, such as combined medications or surgery.
Age influences treatment tolerance and options. Older patients or those with systemic health issues like diabetes or cardiovascular disease may require careful selection of treatments to avoid side effects or drug interactions.
How a patient responds to initial therapies guides further management. If eye drops or laser therapy fail to adequately lower IOP, doctors may recommend surgery or newer treatment modalities.
Treatment adherence is critical for glaucoma management. Eye doctors consider a patient’s daily routine, ability to apply eye drops consistently, and willingness to undergo surgery. Some patients prefer less invasive options even if slower acting.
Patients with rapidly progressing glaucoma or advanced optic nerve damage require more intensive treatment to prevent vision loss. Regular monitoring helps adjust treatment plans promptly.
Availability of specialized glaucoma care, affordability of medications, and proximity to eye clinics can influence treatment choice, especially in regions like Ho Chi Minh City, Vietnam.
By evaluating these factors, eye care professionals can recommend personalized glaucoma treatments that maximize safety, effectiveness, and patient satisfaction. Regular follow-up is essential to adjust therapy as needed and preserve long-term vision.
Glaucoma is often called the “silent thief of sight” because it typically develops without noticeable symptoms in its early stages. By the time vision loss occurs, the damage to the optic nerve is usually permanent. That’s why early detection through regular eye exams is essential to protect your vision and prevent irreversible blindness.
A comprehensive glaucoma screening includes:
Most adults should have a complete eye exam every 1–2 years, or more frequently if they are at high risk for glaucoma. In Ho Chi Minh City, many eye clinics offer glaucoma screening as part of their routine eye care services.
Regular eye exams are the most effective way to detect glaucoma early and prevent vision loss. If you are at risk, don’t wait—schedule a comprehensive eye check with a qualified ophthalmologist.
Although glaucoma is a chronic eye disease, many people live full and active lives with proper management. After diagnosis, protecting your vision becomes a lifelong priority. Following your treatment plan and making healthy lifestyle choices can help slow disease progression and preserve your sight.
Even with treatment, glaucoma can progress. Be aware of signs like:
Living with a chronic eye condition can affect mental health. Don’t hesitate to:
Managing glaucoma is a team effort between you and your eye care provider. With consistent treatment, regular monitoring, and a healthy lifestyle, you can maintain your quality of life and protect your vision for the long term.
If you or a loved one has been diagnosed with glaucoma—or you’re at risk and need screening—choosing the right eye care provider is essential. In Ho Chi Minh City, Vietnam, there are many options, but it’s important to find a clinic with experienced ophthalmologists, advanced diagnostic equipment, and personalized care.
European Eye Center – Trusted Glaucoma Care in HCMC
Located in District 2, European Eye Center is a highly respected clinic offering high-quality glaucoma diagnosis and treatment. Led by Dr. JD Ferwerda, a Dutch-trained ophthalmologist with over 30 years of experience in Europe and Vietnam, the clinic is known for its professional standards, modern equipment, and patient-centered approach.
At European Eye Center, patients benefit from:
You should consult a glaucoma specialist in Ho Chi Minh City if:
European Eye Center is conveniently located and easily accessible for residents and expatriates living in Ho Chi Minh City. The clinic offers English-speaking services and transparent consultations to ensure you feel confident in your treatment plan.
Don’t wait until symptoms appear—book a glaucoma screening today at a trusted clinic like European Eye Center to protect your vision for the future.

In the world of ophthalmology, 20/20 vision is a familiar term, often considered the gold standard for healthy eyes. But

Swimming is one of the most beloved physical activities, offering both stress relief and overall health benefits. However, for those

Myopia, commonly known as nearsightedness, has become an alarming global issue, especially myopia in children. Over the last few decades,

Do you wear contact lenses regularly and sometimes enjoy relaxing with an alcoholic drink? You might have experienced the uncomfortable

In the digital age, our eyes are facing an unprecedented battle. Blue light from screens, UV rays from the sun,

In recent years, a strong global trend has been emerging: medical tourism, also known as health tourism. This involves patients